Choosing the right orthopedic implants is critical in maxillofacial and trauma procedures. How to choose orthopedic implants for maxillofacial and trauma procedures is not a simple question. It requires careful consideration of various factors.
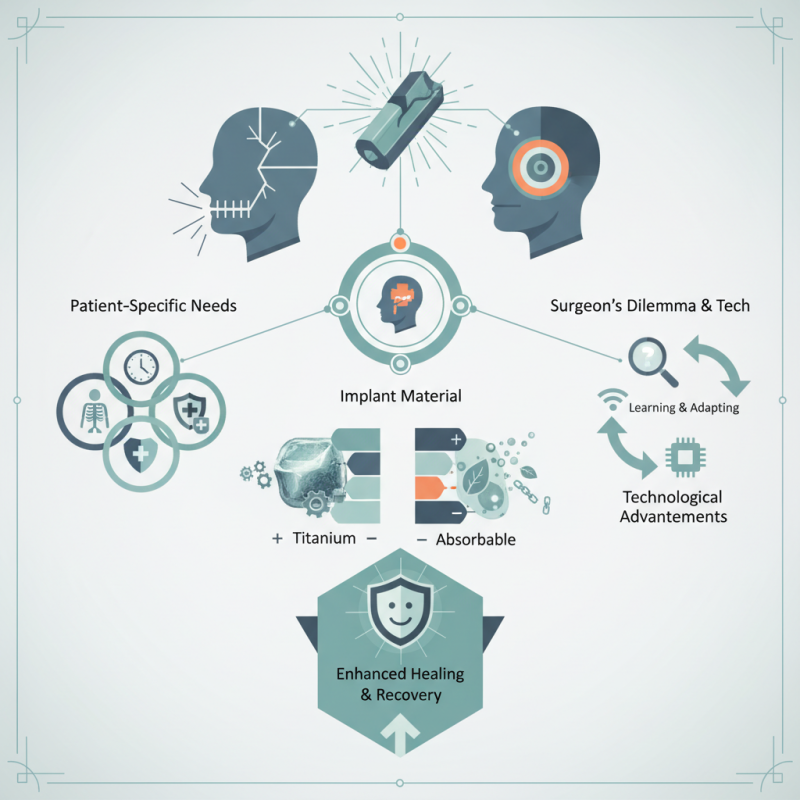
Surgeons must evaluate the patient's specific needs. Each case is unique, influenced by anatomy, age, and health conditions. The implant material is also crucial. Titanium and absorbable implants have distinct advantages and drawbacks. An appropriate choice can significantly enhance healing and recovery.
Surgeons sometimes face dilemmas when selecting implants. What works well in one scenario may not be suitable in another. It is essential to learn from each case and adapt strategies accordingly. Continuous advancements in technology further complicate decision-making. Being informed about the latest options is key. Balancing safety, functionality, and patient comfort is an ongoing challenge that requires reflection and adjustment.
Choosing the right orthopedic implants for facial trauma is crucial. Several key factors come into play in this decision. Material selection is vital. Titanium implants, for instance, offer excellent biocompatibility and strength. However, their higher costs can pose challenges for some patients.
Surgeons must also consider the implant design. Plates and screws need to fit the patient's anatomy precisely. A misfit can lead to complications like infection or poor healing. According to a recent report by the Orthopedic Trauma Association, around 15% of surgeries require revision due to improper implant selection.
Surgeons often face dilemmas during the selection process. Personal experience and preference can influence choices. Yet, evidence-based guidelines are critical. A comprehensive review of clinical outcomes can aid in making informed decisions. In this evolving field, continuous education is vital for improving patient safety and outcomes. Understanding the nuances of each factor is essential for optimal treatment.
| Factor | Description | Importance Level |
|---|---|---|
| Material Type | Implants can be made from titanium, stainless steel, or absorbable materials. Each has unique properties affecting biocompatibility and strength. | High |
| Biomechanical Properties | The ability of the implant to withstand stress and load during healing is crucial for the success of facial trauma repair. | High |
| Size and Fit | Proper sizing ensures that the implant fits well within the anatomical structure, minimizing complications. | Medium |
| Surgical Technique | The ease of implantation and compatibility with surgical techniques can impact the choice of implant. | Medium |
| Regulatory Approval | Ensuring that the implant has proper regulatory approval for safety and efficacy is essential prior to selection. | High |
| Patient-Specific Factors | Considerations such as patient age, health status, and specific anatomical differences are crucial in selecting the correct implant. | High |
When considering orthopedic implants for facial and cranial reconstruction, various types play crucial roles.
Titanium plates and screws are frequently used. They offer strength and biocompatibility, essential for recovery. However, patient reactions to these materials can vary. Some may experience discomfort, requiring close monitoring.
Another option is absorbable implants, often made from polymers. They provide temporary support and gradually dissolve over time. This may reduce the need for a second surgery. Still, their strength may not match that of metal implants. Surgeons need to assess individual cases carefully.
Custom-made implants have gained popularity too. They can be designed to fit the unique contours of a patient’s face.
However, the manufacturing process can be time-consuming. Communication with the patient is vital, ensuring expectations align with surgical outcomes. Decisions should be guided by both the surgeon’s expertise and the patient's specific needs.
When selecting orthopedic implants for the face, material properties are crucial. Titanium and its alloys lead the market thanks to their strength and lightness. According to a recent report, more than 70% of surgeons prefer titanium for facial implants. The metal's corrosion resistance is a key advantage, ensuring longevity in the body. Some also favor polymethyl methacrylate (PMMA) for its ease of use during surgery. PMMA can provide an immediate aesthetic improvement, although it lacks the biomechanical strength of metals.
Biocompatibility is another vital factor. Implants must integrate well with human tissue. Research indicates that titanium exhibits excellent biocompatibility, promoting osseointegration. However, not every patient reacts positively. As per industry data, allergic reactions occur in approximately 3% of patients with titanium implants. In contrast, PMMA can lead to fibrous encapsulation, impacting its function over time. Surgeons face the challenge of balancing material properties with the individual patient’s needs. A personalized approach is often necessary, testing new materials and technologies. The road ahead requires ongoing research to refine these choices.
When selecting orthopedic implants, understanding success rates and complications is crucial. According to a study published in "Journal of Craniofacial Surgery", implants show an overall success rate of 85-90% in facial surgeries. However, complications can arise. Infection rates, for instance, vary from 1% to 5%, depending on the implant material used.
The type of material directly affects these outcomes. Titanium implants generally have a lower complication rate due to their biocompatibility. Conversely, absorbable materials may show a higher incidence of complications, particularly in specific patient populations. Therefore, consult with your surgeon about the potential risks associated with each material.
Tips: Always discuss your specific needs with a surgeon. Ask about their personal success rates with different implants. It's essential to understand the intricacies of your case. Monitor post-operative symptoms closely. Early detection of complications can significantly improve outcomes. Make informed choices based on reliable data and expert guidance.
When it comes to orthopedic implants for facial and trauma cases, customization is key. Selecting the right implant requires a deep understanding of each patient's unique anatomy. Many times, standard implants simply do not fit well. An oversized implant can lead to discomfort. An undersized one may fail to provide necessary support. This variability highlights the importance of precision in measurements.
Consider the patient's bone structure and the specific area needing repair. Each face is different; the contours vary. Imaging technology can provide a detailed view of the anatomy. However, these images may not capture minute details. Surgeons must rely on both their skills and their experience. Sometimes, this means adjusting the implant design during surgery based on real-time observations.
The process can be intricate. Implants created using 3D printing technology are gaining traction. They offer tailored solutions but require careful planning. Still, misjudgments can occur. Surgeons may find that the implant does not align perfectly with the bone. This can lead to complications in healing and function. Reflection and adaptability during the procedure are essential in these scenarios.
: Titanium and its alloys are preferred due to their strength and lightness. PMMA is also used for its ease during surgery.
Biocompatibility ensures implants integrate well with human tissue and function properly over time.
Titanium shows excellent biocompatibility and promotes osseointegration, aiding in secure placement.
Yes, about 3% of patients may experience allergic reactions to titanium implants.
The success rate ranges from 85% to 90%, depending on various factors, including material choice.
Titanium generally has lower complication rates, while absorbable materials may lead to more issues in certain patients.
Patients should review specific needs, potential risks, and the surgeon's success rates with different implants.
Close monitoring of post-operative symptoms is vital for early detection of complications and improved outcomes.
Continuous research helps refine material choices and improve safety and effectiveness for individual patients.
PMMA can provide immediate aesthetic improvements, making it appealing, despite lower biomechanical strength and function risks.
Choosing the right orthopedic implants for maxillofacial and trauma procedures is crucial for successful patient outcomes. Key factors to consider include the specific anatomical needs of the patient, the types of implants available, and their material properties and biocompatibility. Several types of orthopedic implants are utilized in facial and cranial reconstruction, each with varying success rates and potential complications.
Understanding these elements helps in customizing implants that cater to the unique requirements of individual patients. By thoroughly evaluating the available options and considering the success rates associated with different implant types, healthcare providers can enhance the quality of care and optimize the healing process for patients facing facial trauma. Thus, an informed approach to "how to choose orthopedic implants for maxillofacial and trauma procedures" is essential for effective treatment.

 Voila Orthopedic Implants
Voila Orthopedic Implants